Candida Subspecies: Albicans, Tropicalis, Glabrata, Krusei, Parapsilosis
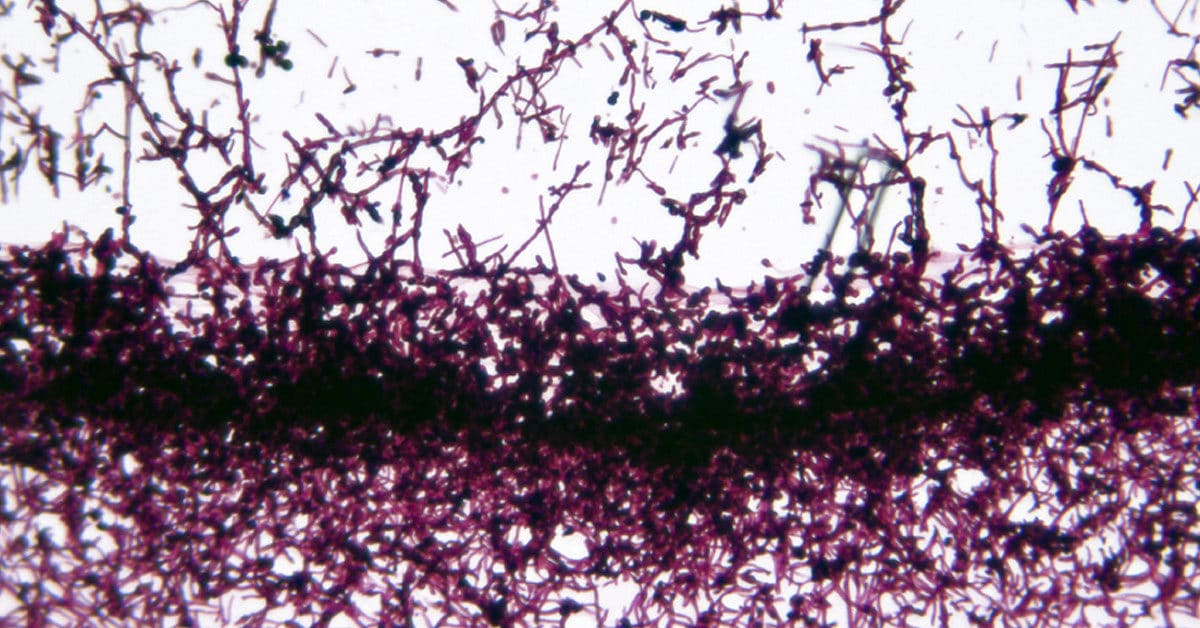
Many people struggling with yeast infections or gut dysbiosis often just refer to themselves as just having a problem with ‘Candida.’ But in reality there are over 150 subspecies of Candida! Thankfully only 6 are typically associated with problematic infection in humans. These are:
- Candida albicans: by far the most commonly known, typically accounting for about 50% of cases around the globe;
- Candida tropicalis: accounting for 15-20% of cases. Not usually as aggressive as Candida albicans;
- Candida glabrata: accounting for 15-20% of cases;
- Candida parapsilosis: accounting for 15-20% of cases, especially in Europe;
- Candida krusei: a rare species, usually only around 1% of cases, especially in infantile diarrhea and occasionally systemic candidiasis;
- Candida lusitaniae: another rare species type, usually involved in septicemia and/or pyelonephritis cases.
Many factors go into determining whether the presence of a Candida species will cause a person any trouble. The first and most important question is, “How healthy are you overall?” Your lifestyle choices (for example eating well, resting, exercising, avoiding toxins, etc.) go a long way to determine the strength of your immune system and your ability to fight off Candida infections. Supporting a healthy immune system is key to keeping any opportunistic infection at bay, and this is very much the case with Candida too.
Table Of Contents
Some Types Of Candida Are More Virulent Than Others
Each of these species has a particular set of properties, meaning that some are much more virulent than others. We can evaluate their particular virulence and potential for infestation by looking at a few key factors. These include:
- Their potential to form hyphae (i.e. invasive, finger-like projections that invade tissue and deeply root the infection). Three primary species do this: Candida albicans, Candida tropicalis, and another type called Candida dubliniensis;
- Their potential to upregulate biofilm creation, which is a spider-web like matrix where yeast and other microorganisms are shielded from your immune system. Candida krusei and Candida tropicalis are the most capable of subspecies in this regard.
- Their potential to produce phospholipase, a fatty acid-dissolving enzyme that allows the species to infiltrate host cells, adhere to them, and penetrate deeply. Candida albicans produces the highest levels of this enzyme.
- Their potential to produce proteinase, a protein dissolving enzyme that functions in a similar way to the phospholipase. Again, Candida albicans produces highest amounts of this.
How Can You Tell Which Candida Subspecies Is Causing You Trouble?
The best way to diagnose which Candida subspecies is causing your symptoms (such as yeast infections, digestive complaints or other issues) is by getting a diagnosis by stool test. A thorough analysis of your stool will identify pathogenic bacteria and a number of other factors that might be causing problems, in addition to including a yeast culture to look for Candida.
Candida albicans is by far the most common variant of Candida, but the particular type that you are suffering from depends on a number of factors. Geographic location is one example, and indeed Candida parapsilosis is found much more often in Europe.
Another factor is the strength of your immune system and any other conditions that you may have. For instance, Candida glabrata is most likely to affect those battling AIDS, and is therefore responsible for a higher mortality rate than any other species of Candida. If patients are given Diflucan over long periods of time, they can be susceptible to resistant strains like Candida krusei. Lastly, Candida parapsilosis is also often found in immune-weakened individuals and is highly resistant to antimicrobial drugs.
You should also be aware of Candida auris, a rare but extremely virulent subspecies of Candida that can be life-threatening in patients with weakened immune system. Candida auris has developed resistance to a number of prescription antifungals, and has proven extremely difficult to treat. It is usually found in hospital settings and can be passed from one person to another, often via healthcare workers.
What Should You Be Looking For?
So what should you be most concerned with then when it comes to these various types of Candida? First of all, think about any other health issues that you may be struggling with.
The overall virulence of particular strains depend on many things, including pre-existing conditions, your overall level of immunity, the site where Candida is introduced and the stage of infection. Catching it early can make a big difference in how hard it is to clear.
Furthermore, your current medication regime can considerably impact your risk factors. For instance, if you are on an immunosuppressant medication like a steroid, you may want to be especially mindful that a Candida krusei infection could develop.
If you can’t identify any particular factors relating to your immune system or medication, it is most likely that you have a Candida albicans infection. Candida albicans is present in a high proportion of cases and as one of the most aggressive types.
If you think its likely that your Candida is caused by one of the types that creates strong biofilms (e.g. krusei or tropicalis), that will have implications for your most effective treatment options. For example, you might want to consider using a supplement that disrupts biofilms, like nattokinase or lumbrokinase. In the Ultimate Candida Diet, Dr Eric Wood and I discuss biofilm-disruptors like these in much more detail, and lay out a plan for when you should introduce them to your treatment.
Ultimately, the foundation of treatment for most of these Candida infections comes down to three main elements, irrespective of which subspecies you have. Take a good probiotic to repopulate your gut, use antifungals to destroy the Candida cells, and follow a low sugar diet plan to deny the Candida colonies the food they need to expand and grow.

3-Month Candida Elimination Kit Start Your 3-month Candida Cleanse
This Candida Kit contains all the supplements recommended on the Candida Diet:
- LIVER ONE to process and remove the toxins created by Candida.
- CANDASSIST to inhibit and weaken the Candida colonies in your gut.
- PROBIOTIC to replace the Candida yeast with probiotic bacteria.
Plus... the CANDIDA DIET RECIPE BOOK with 50+ low-sugar recipes


Wow! I never knew there were subcategories. You mention getting a stool test in order to confirm which we’re dealing with. Can you please advise as to what that test is called. Does one need a prescription for it? Will any lab be able to perform this test?
Candida Krusei is what I was diagnosed, and as you said is one of the types that creates strong biofilms, and that will have implications for my most effective treatment options. For example, I will consider using a supplement that disrupts biofilms, like nattokinase or lumbrokinase. I was dx in 2010 with 3+ and again in 2014 with 1+. Do you have any other suggestions?
Have you found a treatment that works? It is really a rare one and there’s
no cases on the web for treating it in the gut, just blood-borne cases.
Hi! I have candida krusei also and looked up essential oils that help it. I lost the paper I wrote everything down on but I did a quick search that led me back to the Body Ecology website. They have some good info there on how clove oil and lemongrass oil break down biofilm. I did this search a few weeks ago but just remembered that I was excited when I realized the oils that seemed best after lots of research were all in Thieves oil by Young Living. I’m not sure why I didn’t start using it regularly (brain fog maybe?). Those oils are clove, lemon, cinnamon, and Rosemary. Hope this helps!
I am 5’7″ and now 105 lbs. How do I not lose weight and gain weight?
I also am conscious of how acidic my body has been (bones feel like glass and teeth were disintegrating). So, true Paleo is hard. Starch based is hard. lol. Too much fat and I feel pains in where my breast cancer was and my fibroid hurts/sore.
How do I gain weight?
🙂
Foods like coconut oil, eggs and avocado are good options for those trying to gain weight on the diet. Also make lots of coconut bread!
Are there different treatments depending on types of Candida? Otherwise I do not understand why I need to check which type I have. In my case I have big problems with my skin. Ordinary treatment (both cortison and other treatments) has had no impact for many years, treating Candida has made much bigger improvements. In my case Candida in my skin has been like an entrance for other viruses or bacteria, or the other way around. But the doctors do not believe this.
The type of Candida that you have can affect the way that you treat it, for example those subspecies that are particularly liable to create biofilms.
I had a really bad candida skin problem for several years until last year I gave up any form of sugar, (no sweetners either), including most fruit (I take vit c caps),and some veg, also no yeast and I eat a GF low carb diet, I used AloeVera gel to stop the itching and the infection has largely disappeared, only an occasional pinpoint flareup if I cheat on my diet. I am hoping that in time the Candida will die off completely and I can reintroduce some fruit. I didn’t know about the different types of Candida so am now going to investigate a bit to see if I can find out which I had. An allergy specialist did give me a stool test but I found out afterwards that it was only used to determine if I had parasites!
I doubt you can just reintroduce fruit. If you’ve followed a low carb diet, the typical candida diet, then adding fruit will cause a flair up.
To add fruit back in you need to do an anti-candida diet, so that any excess sugars in th blood are quickly mopped up, leaving the candida with nothing to feed upon.
I have been diagnosed( swab test) with Vaginal Candida glabrata( tested negative for HIV and Diabetes, haven’t been on contraceptive or antibiotics either). I have been following your protocol and am now at the stage to introduce antifungals. I am wondering which of these antifungals specifically work for candida glabrata? I don’t want to invest in an antifungal which only affects candida albicans. Can you please advise?
I have Candida Glabrata and have been on Flucytosine tablets for almost a month now, and have just started using Nystatin and following the guidelines to this diet. I started taking Fem Dophilus probiotics, as well, and those have really done wonders. I feel a lot better than before, but it’s definitely triggered by some foods, I can tell. I’ve only known about my Glabrate for a couple months now, so it hasn’t been very long at all. I’m hoping change of diet and lifestyle will get rid of this thing! Good luck to you, hopefully you’ve figured it out by now (since it’s been 9 months since you last posted).
I just found out that I have Glabrata. Where do I find out info on this? Is it contagious? What about my husband? Can you explain more about diet?
How did you get diagnosed with glabrata? I have yeast symptoms. Discharge, itchyness, redness and burning. My tests came up with yeast two months ago and I took Diflucan and creams. Nothing worked. Symptoms never went away. I got tested twice again and now yeast isn’t coming up at all! I don’t know what to do!
I was diagnosed with Candida Krusei last week after having diarrhea for 40 days. My natural doctor gave me a lot of natural things to take and it is working but the die off is something else. I also have a very sore mouth right now after about a week into treatment. Any ideas on that?
I was diagnosed too with c. krusei. I’ve vaginitis and it came after having diarrhea for 6 days, stomach pain ad feeling very week. Couldn’t even eat. Dr gave me antibiotics for only 3 days, to stop diarrhea and then it started burning… My stomach in now ok, but down there…no.
I was diagnoses with Candida Krusei and my NP did a sensitivity panel on the stool culture which said I should take Plant Tannins & Uva-Ursi. I also take an enzyme to break down the bio film. The culture was done 4 months after I started the Ultimate Candida diet- which I truly believe saved my life. We can only wonder how infected I was before the diet! I still follow the diet on most days, but am less strict since I started feeling so good. All those nasty symptoms went away. I rarely eat sugar and fruit yet, and very little starchy veggies. No bread or gluten products. If you follow this diet, you can really support your liver through the die-off.
Do you have anymore information on Candida Dubliniensis? I did a stool test and it was that species that was found in my stool.
I am 18, and I was recently diagnosed with Candida Krusei, I have tried everything. And since it is so rare, there is hardly enough info on how to treat it online. I am starting to think it has become very resistant to the medication, due to the fact that for weeks I was given diflucan which krusei is resistant to it. They didn’t know what I had and even ruled it as a STD when I’ve never even had sex. I finally went to an OBGYN and that’s when I found out I had Candid Krusei. I was given another medication, which seemed to work but the symptom soon came back. And now it has been approximately 4 months that I have had to deal with this. Can someone please help, I am tired of being in pain 🙁
Hi Grace, have you tried a low sugar diet, natural antifungals and probiotics? You might find that they help.
My 15 year old has been having bad stomach pains, diarrhea for over a year. She was diagnosed with Colitis but once her calprotetin levels came down the GI doctor said Sayonara. And dropped us as being cleared of colitis. With her in stomach pain every single day and barely eating for months i went to a naturopathic doctor.
She did a stool sample our GI doctor never did and confirmed Candida Krusei. My daughter is being treated with Naturopathics called CandidaSTAT. It has the stuff that c.krusei is susceptible to in it. We were provided with a list of Natural Antifungals:
Berberine
Caprylic Acid
Uva Ursi
Plant Tannins
Grapefruit Seed Abstract