What Are Candida Biofilms?
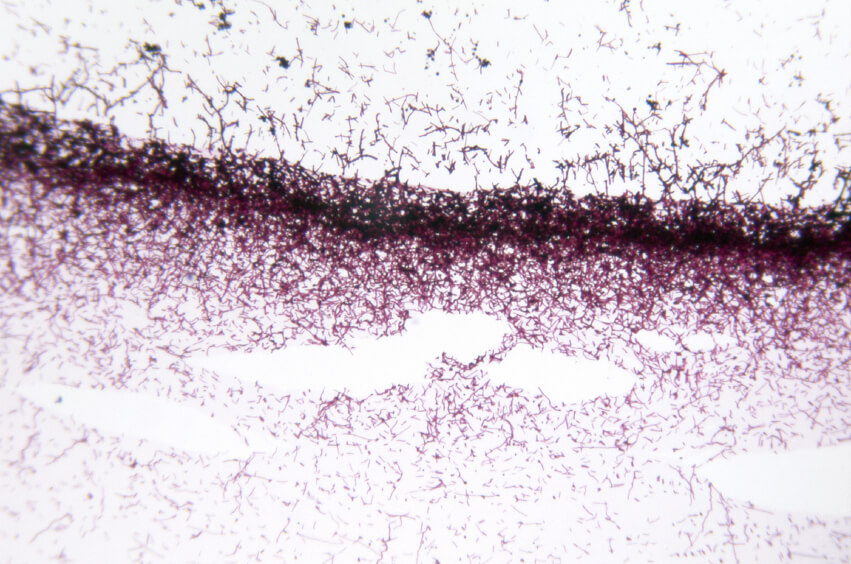
Candida biofilms are complex, protective structures formed by Candida species, particularly Candida albicans. These biofilms are made up of dense microbial communities encased in a polysaccharide matrix, which acts as a shield against external threats, including antifungal treatments and the immune system.
Biofilms allow Candida to persist in harsh environments, contributing to the difficulty in treating Candida infections effectively.
Table Of Contents
Supplements to Fight Candida Biofilms
A wide range of natural remedies can be used to destroy Candida biofilms, which may help to prevent Candida overgrowth. Many of these have been used in traditional medicinal practices for centuries, but have also recently been clinically tested as effective solutions.
Oregano Leaf Extract
- Powerful antifungal: Oregano leaf extract is renowned for its ability to inhibit a variety of pathogens, including Candida yeast. Its active ingredient, carvacrol, is rich in phenols that effectively attack and break down biofilms.
- Prevents resistance: Unlike other antifungal agents, Candida does not easily develop resistance to oregano leaf extract, making it a reliable long-term option for prevention and treatment.
Oregano leaf extract showed significant antibacterial activity against 11 biofilm-forming microbes, including four methicillin-resistant Staphylococcus aureus (MRSA). Most importantly, oregano leaf extract was found to effectively break down the biofilms formed by each of these pathogens.
Carvacrol has been found to inhibit a range of antibiotic resistant bacteria, viruses, parasites, and fungi. Its inhibitory effect extends to preventing these toxins from releasing harmful substances and forming biofilms.
Candida yeast doesn’t appear to become resistant to oregano leaf extract, which can happen with other antifungal agents.
Supplements with oregano leaf extract are generally available in capsule form at most health stores. You can also check out our recommended CandAssist supplement, which contains a number of the antifungals on this page.
Caprylic Acid
- Biofilm penetration: Derived from coconut oil, caprylic acid can penetrate and eradicate persistent Candida biofilms within just 60 minutes of exposure.
- Broad-spectrum action: In addition to Candida, caprylic acid is effective against other harmful bacteria like MRSA and E. coli, offering wide-ranging benefits for gut health.
Caprylic acid is the active antifungal constituent of coconut oil. As well as its many other health benefits, substantial research has suggested that caprylic acid has an ability to penetrate and eradicate persistent Candida biofilms.
A study published in Frontiers in Microbiology showed that a combination of caprylic acid and soluble fiber was able to eliminate pathogenic biofilms within 60 minutes of exposure without causing harm to the surrounding healthy cells.
As well as destroying Candida biofilms, caprylic acid has been found to inhibit MRSA (methicillin-resistant staphylococcus aureus), as well as E. coli, Salmonella and P. aeruginosa bacteria.
Garlic
- Potent biofilm disruptor: The allicin in fresh garlic is highly effective against Candida biofilms, even in cases where other treatments fail. Research highlights its superiority over garlic powder in disrupting biofilm growth.
- Long-term protection: Regular use of fresh garlic can prevent the formation of biofilms, making it a strong candidate for ongoing Candida management.
The allicin content of fresh garlic is a sulfuric compound that has powerful activity against both bacteria and fungi. Research has shown that it’s particularly effective against Candida biofilms, even those with increased resistance to other natural antifungal agents.
Interestingly, another study showed that fresh garlic extract is much more effective than garlic powder extract in treating Candida. Although dried garlic can eradicate Candida to some extent, fresh garlic provides a much broader activity against the morphology and growth of the Candida yeast.
If using garlic as part of your Candida treatment regime, avoid cooking it for longer than five minutes as heat will destroy its therapeutic properties. It’s also better taken with a little healthy fat (such as olive oil or coconut oil) as crushed garlic can burn sensitive membranes.
Like oregano oil, Candida is unlikely to develop a resistance to garlic, which makes it a promising option for long-term prevention.
N-Acetyl Cysteine (NAC)
- Biofilm weakening: NAC is a powerful supplement that weakens and breaks down the biofilm matrix, reducing Candida’s ability to adhere to surfaces by over 32%.
- Combination therapy: When used with antifungals like ketoconazole, NAC can lead to the total eradication of tough Candida biofilms, offering a comprehensive treatment approach.
Studies have shown that NAC can reduce Candida albicans adherence by more than 32%. This is especially impressive when compared to pharmaceutical drugs such as ketoconazole, which typically reduce Candida growth by only around 25%. NAC is also found to have a more potent disruptive effect than ketoconazole (22-80.7%) on mature biofilms.
NAC and ketoconazole are particularly useful when used together, showing total eradication of tough Candida biofilm. At the same time, NAC has been found to prevent further growth and replication of Candida, which is an important step in biofilm formation. It’s also able to change the texture of the biofilm, making it easier to break down.
Higher concentrations of NAC are more effective, as well as combining NAC with other antifungals.
Systemic Enzymes
- Whole-body support: Systemic enzymes, like serrapeptase and nattokinase, are not only effective at breaking down biofilms but also support overall body health by reducing inflammation and improving circulation.
- Versatile use: These enzymes have shown promise in treating various biofilm-related conditions, including those associated with Lyme disease, suggesting potential broader applications for Candida management.
Good examples of systemic enzymes are serrapeptase and nattokinase. These two proteolytic enzymes have been shown to inhibit biofilm formation, which can make them an incredibly useful addition to any Candida treatment plan. These systemic enzymes are proven biofilm disruptors, and not just for Candida albicans.
Research has suggested that systemic enzymes may be useful for breaking down the biofilms associated with Lyme disease. This has raised the possibility of treating Candida biofilms in the same way. More research on using systemic enzymes for fungal infections is pending.
If you’re interested in using systemic enzymes to treat a yeast overgrowth, check out our SerraDefend formula. This formula contains the two systemic enzymes serrapeptase and nattokinase. It also contains a group of digestive enzymes chosen for their ability to break down yeast cell walls and inhibit biofilm formation.
How Are Candida Biofilms Formed?
While the process is complex, we can distill Candida biofilm formation into 5 key steps.
- Initial Adhesion: Individual Candida yeast cells attach to a surface such as the tissue in your gut wall..
- Cell Multiplication: Once attached, the yeast cells begin to multiply, increasing the number of cells at the site.
- Extracellular Matrix Production: The multiplying cells produce an extracellular matrix, primarily composed of polysaccharides. This matrix holds the cells together and anchors them to the surface.
- Protection Development: The extracellular matrix creates a protective barrier that shields the Candida cells from antifungal agents and the immune system.
- Biofilm Maturation: As the biofilm matures, it becomes a highly organized structure. Different cell types, including yeast, hyphal, and pseudohyphal cells, form within the biofilm, each playing a role in maintaining its integrity and function.
Health Significance of Candida Biofilms
Candida biofilms play a significant role in the persistence and severity of Candida infections. These biofilms are often found in the gut, or on medical devices like catheters, heart valves, and prosthetic joints, where they can lead to severe, chronic infections resistant to treatment.
The protective matrix makes it difficult for antifungal drugs to penetrate and kill the Candida cells within, leading to recurrent infections and prolonged illness.
The biofilm’s ability to resist treatment is particularly concerning in immunocompromised individuals, such as those undergoing chemotherapy or living with HIV/AIDS. In these patients, Candida biofilms can cause life-threatening systemic infections that are challenging to manage.
Moreover, the presence of glucose in the matrix composition highlights the role of sugar in biofilm development, suggesting that dietary factors may influence the persistence of Candida biofilms.
Candida Biofilms Symptoms & Causes
Biofilms are present in almost any Candida infection, so the symptoms of Candida biofilms are much the same as the symptoms of Candida overgrowth.
Symptoms of Candida Biofilm Infections:
- Chronic Fatigue
- Brain Fog
- Digestive Issues
- Recurring Yeast Infections
- Oral Thrush
- Sinus Infections
- Food Sensitivities
- Fungal Infections On The Skin And Nails
- A Weak Immune System
- Joint Pain
- Low Mood
Causes of Candida Biofilm Formation:
- Weak Immune System: Individuals with compromised immunity are more susceptible to biofilm-related infections.
- High Sugar Diet: Excessive consumption of sugar and refined carbs feeds Candida, aiding biofilm development.
- Antibiotic Use: Prolonged antibiotic use disrupts the balance of bacteria, allowing Candida to overgrow and form biofilms.
- Stress and Hormonal Imbalances: Both can weaken the body’s defenses, making it easier for Candida to thrive and form protective biofilms.
Quick & Easy Tips to Prevent Candida Biofilm Formation
- Optimize your diet: Limit sugar, refined carbs, and yeast, which feed Candida. Focus on a low-sugar diet rich in vegetables to starve biofilms.
- Use natural antifungals: Caprylic acid, berberine, and oregano oil are potent, natural antifungals. They disrupt biofilms and prevent Candida from thriving. Add these to your routine for effective prevention.
- Incorporate probiotics: Probiotics like Lactobacillus rhamnosus can help balance your gut microbiome, reducing the chances of Candida forming biofilms.
- Stay hydrated: Drink plenty of water to flush out toxins and prevent biofilm formation. Aim for at least 8 glasses daily.
- Manage stress: High stress weakens your immune system. Practice stress-reduction techniques like meditation or exercise to keep Candida in check.
Breaking A Candida Biofilm
There is no simple way to destroy a Candida biofilm in your gut. For the most part biofilms do exactly what they are designed to do – protect the Candida albicans cells from your immune system. There is no magic pill we can take to immediately eliminate a Candida biofilm. It takes time and application.
Why Are Candida Biofilms Difficult to Treat?
Biofilms are one of the main reasons why a Candida overgrowth is so hard to beat.
A longstanding Candida overgrowth has had plenty of time to create biofilms in your gut. These are very resistant to many of the treatments we can throw at them. The longer the biofilm has had to develop, the more resistant it will be to antifungal treatments.
This is why using antifungals alone is often not enough to beat a Candida overgrowth. We need to adopt several different strategies.
Try Our Candida Treatment Plan
Our Candida treatment plan, the Ultimate Candida Diet, uses several different elements to fight Candida. These include antifungals, probiotics, and a low-sugar diet. We also discuss the use of systemic enzymes, such as serrapeptase, which have been shown to break down biofilms such as those created by Lyme, Candida, and other infections.
Adding these systemic enzymes to your treatment can make your probiotics and antifungal therapies much more effective.
Used alone, these strategies will likely fail. But used together, they can be highly effective.
The antifungals destroy the cell walls of the Candida; the enzymes break down the biofilms; the probiotics support your immune system and regulate the acidity in your gut; and the low-sugar diet deprives the Candida of the resources that it needs to grow. This combination of treatments is much more effective than using a single strategy.
FAQs
How to Get Rid of Candida Biofilm in the Gut?
Start by incorporating antifungal agents like oregano oil and caprylic acid, which are known to penetrate and disrupt biofilms. Combine these with a low-sugar diet to starve Candida of its primary food source. Consistency is key to eradicating the biofilm completely.
What Foods Break Down Candida Biofilms?
Garlic, coconut oil, and oregano are potent biofilm disruptors. Fermented foods like sauerkraut and kimchi also help by promoting healthy gut bacteria, which can outcompete Candida.
Is Candida Albicans Contagious?
Candida albicans can be contagious in certain situations. It can spread through direct contact, such as during childbirth, kissing, or sexual activity. Maintaining good hygiene and treating infections promptly reduces the risk of spreading Candida.
Can You Fully Remove Candida Biofilms?
Yes, but it’s challenging. Fully removing Candida biofilms involves using a combination of antifungal treatments, a low-sugar diet, and possibly the inclusion of systemic enzymes that target and dismantle the biofilm structure. Persistence is essential, as biofilms are highly resistant and can take time to fully eliminate.

3-Month Candida Elimination Kit Start Your 3-month Candida Cleanse
This Candida Kit contains all the supplements recommended on the Candida Diet:
- LIVER ONE to process and remove the toxins created by Candida.
- CANDASSIST to inhibit and weaken the Candida colonies in your gut.
- PROBIOTIC to replace the Candida yeast with probiotic bacteria.
Plus... the CANDIDA DIET RECIPE BOOK with 50+ low-sugar recipes

Hi Lisa good to get updates on the Candida albicans bio films @ how to treat them, this whole candida problem, especially earlier on when I didn’t understand it @ how to combat it was driving me crazy with the toxin release@ anxiety problems, thank you for your help.
How did you treat yours? I’m new to this still doing research I haven’t been able to find a naturopathic doctor just yet but I’m desperate at this point so I went to natural foods and bought some things that I thought might help with the help of the store clerk. I need advice because she told me that I am magnesium deficient and gave me magnesium supplements for my anxiety it’s in the form of a powder you can put in water. I also have Candida support intestinal health supplements it has Pau D’Arco, oregano oil, black walnut, and caprylic acid in it, other ingredients contain (cellulose for the capsule, garlic bulb, olive leaf, cat’s claw root, wormwood herb, silica, magnesium stearate, and cellulose power). Fem dophilus probiotic capsules with just lactobacillus rhannosus, GR-1, lactobacillus reuteri, RC-14 plus other added ingredients like (dextrose and anhydrate potato starch cellulose and magnesium stearate) (capsules consists of gelatin and titanium dioxide) also Dairy casing in trace amounts, virgin olive oil, vegetarian fruitein high protein energy shake rainbow from Nature plus. It has a vast amount of ingredients as well as multivitamins including magnesium 200 milligram which is 50% of the product. Did I make the right choices?? I’m so clueless and in need of serious help I feel like this is killing me! I started experiencing severe symptoms almost instantly started off with anxiety and panic attacks. I’ve had a fungal infection on my skin for some years now and recurring yeast infections and UTIs treated with antibiotics some left untreated sometimes because I was so focused on my mental health I thought I was going crazy last year I was admitted into the hospital and then again this year a few weeks ago for chronic panic attacks I feel like my body is shutting down every morning I wake up with severe heart palpitations feeling faint dizzy basically feel like I’m dying I connected My reoccurring infections and fungus with my anxiety a couple days ago on Google and found candida. And when I seen the systematic symptoms I completely freaked out! Is it too late for me? Am i dying?! I need help!! Please I need advice because it’s been difficult trying to find a doctor that takes government insurance I don’t think anyone does on a naturopathic/holistic level in my state. I will do anything to get better as long as I don’t have to feel this way anymore its ruining my life and I believe it’s killing me and in a rapid pace. Also I’m a hundred and seventeen pounds I’ve always been super skinny I’m 5’9 27 and I have been dealing with reoccurring yeast infections UTI and fungal skin infection since I was about 17 is there any hope for me. I pray everyday for answers
Hi Birdy. I hope you are improving. Felt compelled to write when I saw your post. I stumbled across this site looking for some research for my Dad. I battled and won my fight with candida some years ago, it was a long road with a naturopath but there are more answers and resources on the internet now I think you absolutely can do it yourself – and YOU will get well. I just wanted to wish you all the best in your recovery. X
Get serrapeptase by doctor’s best 40000 spu dose it 3 capsules 2 or 3 times daily. Then another good attack is Biofase. It is an all around candida killer! Bit pricey….but totally worth it! Try very hard to eliminate sugar,…except try buying a natural , no artificial anything, beet juice,…read or listen to Robert Von Sarbacher on YouTube about his mini beet protocol! And, Olive Leaf Extract is powerful fungal killer too. Also, check out information on Berberine hcl, it too is a powerful anti-viral, anti-bacterial, antifungal!
Birdy, I have had very similar issues. There is hope for you!! Don’t despair. Your Candida (which probably has a biofilm) is running interference for the other ailments you are trying to cure. Kill the candida, and you can kill a uti (and others)… For good! I have been plagued with chronic, antibiotic resistant uti’s and have been clearing my body of so much candida/biofilm and things have gotten SO much better. Good luck!
I’d say change your diet to allow the least amount of sugar in your system. I just started my diet a week and a half ago and i am struggling to keep up with it but i need/want to get better. I’m taking probiotics by pill and through Activia yogurts and I’m seeing small improvements but not where i feel comfortable. I will add you to my prayer list . I hope you start to see results soon .
Hi Birdy, Have you ever heard of prime tea from the book called The Prime: Prepare and Repair Your Body for Spontaneous Weight Loss by Kulreet Chaudhary. It worked great for me. The books at Amazon and the tea it’s made from seeds. You boil and drink it every day. It took me a month of drinking it but it did the trick. It also made my good bacteria thrive, my taste buds changed, and I was craving salads and greens. It has 3 little ingredients in it. Coriander, cumin, and fennel seeds. That’s just the beginning of the book. It has more great advice and recipes to help with all the junk that comes with this horrible affliction. The woman who wrote it is a neurologist. I hope you try it. Its soothing. I still use it on a part time basis.
Hi Byrdie-this is 4 years late but were you Floxed? If you took a Fluoroquinolone Antibiotic at any time in the past I would look into Fluoroquinolone Toxicity. Your history & symptoms sound much like mine after taking Cipro for a UTI & that damage it caused me.
This is one of the most important pages on this website! It needs its own category/button, not hidden in an article.
I’d really like to thank the creator of this website for helping me start to understand what has likely been making me so sick.
It has encouraged me to use Google Scholar to find academic research on biofilms (there’s A TON, anti-biofilm medication is a future billion dollar industry). Something tells me that yeast and biofilms are the next “trend”. These biofilms are nasty and from the research, nearly impossible to eradicate. Candida infections have a 15-35% mortality rate, and while I’m assuming this is people in a hospital setting this is still a very scary fact. At anytime someone can be hospitalized/injured and having candida overgrowth significantly raises your chances of complications or death.
I’ve been telling a lot of people about Candida, and it’s typically greeted with “oh that’s not my problem” despite 50-60% of people having Candida overgrowth. It’s one of those things that people just cant wrap their heads around.
Some things that I’m trying that may not be on this site: (no guarantees on these, just trying to help others who are suffering like me)
– Coriander (works on biofilm according to 2015 study)
– Diatomaceous Earth (Food grade DE only, there are other kinds that are used as nontoxic-to-humans insect killer, check out a picture of it under microscope, it is claimed that it tears tiny holes in the yeast cells and I’m hoping that it will act as a “scrub brush” for this extremely stubborn biofilm that your candida is hiding in)
– Bentonite Clay
– pH test strips (to test the pH of my saliva – candida biofilms are in your mouth too grown by acidity..another tip here is to monitor oral biofilms)
– Cayenne pepper
– Bioflavonoids seem to interrupt the ability of cells to communicate with each other, called Quorum-Sensing (this is how the cells know its time to advance to form a biofilm)
– Xylitol the sweetener seems to be an anti-biofilm
– Aspirin (Salicylates) interfere with the biofilm matrix
– Iron
– Bismuth (Pepto Bismol)
– EDTA Chelation (I likely won’t be trying this due to cost and it seems questionable)
– Food Grade Charcoal
– Baking Soda (Planning to eat it too but it an awesome oral anti-biofilm with immediate effects)
– Serrapeptase supplements
– Ludol’s Enema and a Liver Flush
– Kefir Enema
No medication should be taken during candida treatment.The antibiotics is root cause of the candida in first place.No sugar,no calcium,no bread or dairy products should be taken during the course.
I think I have this infection It became worse after 3 rounds of antibiotics from UTI infections. Now it makes sense. I kept telling doctor that my problems got worse after antibiotics, in fact my mouth area burst out with fever blisters from so much acidity in my stomach.
The amino acid, L-Lysine for fever blisters; also, colds, flus, chicken pox, shingles; 4X500mg, twice daily. Twice/day for maintenance.
I think I have this infection It became worse after 3 rounds of antibiotics from UTI infections. Now it makes sense. I kept telling doctor that my problems got worse after antibiotics, in fact my mouth area burst out with fever blisters from so much acidity in my stomach. My GI doctor told me there was NO way I had a fungal infection. I got an endoscopy and colonoscopy and all was clear. He would not test me for fungal infection or offered a stool test.
There are also supplements that can help to break down biofilms. Ideally, these are taken 20-30 minutes before taking antifungals. Some common biofilm disruptors are nattokinase, serrapeptase, lumbrokinase, N-acetylcysteine, selenium and lactoferrin. There are also blends such as Klaire Labs Interfase Plus.
Anything that sounds like a chemical or pharmaceutical scares me to death! 🙁
@ Chae I think that the last 3 ( N-acetylcysteine, selenium and lactoferrin) are amino acid, mineral and amino acid or enzyme, hence, natural. I was taking lactoferrin separately for immune system but it seamed to be not working. Never took it half an hour prior to anti-fungals though.
@ Beth Do you have any links to research studies that have found it?
Cool! Check it out:
http://pubs.sciepub.com/ajidm/2/5/5/
N-acetyl cysteine is also known as NAC, one of the supplements Lisa recommended for the protocol. Already on it… BAM! I know this is an old post, but I’m hoping someone else might benefit from looking at the literature. Way to be a boss, Lisa.
How much NAC do you use? Thanks.
Sorry….used with Nystatin ok?
I realized I had a candida overgrowth six months ago when repeated UTI’s became almost constant. It was wreaking havoc with my relationship and was detrimental to my self-esteem.
I read as much as I could find on the subject, trying to take into consideration all the different approaches in the varied information out there and started implementing changes in my diet. Lisa’s book was the most informative and comprehensive I found; thorough, easy to understand and educational. Once I understood the impact those little microbes had on my system it was a serious effort to clean myself up.
After about two months things were mostly better and I started adding things back into my diet. I wouldn’t say my candida overgrowth is 100% gone, but I no longer need to take the anti-fungals every day and I can have a little of some of the forbidden foods from time to time. I no longer eat trigger foods and don’t think I ever will. I feel so much better and now have the knowledge and understanding of how to deal with this life changing overgrowth if it ever reappears again.
Thank you, Lisa, for the best information I could find anywhere.
Thanks Jen, I’m really glad to hear that you found my program useful 🙂
Lisa, I have been on the Candida Diet for a month. I think things are improving. My situation is that I have Leaky Gut which I began to treat before I became aware that the candida was causing the Leaky Gut. How do I know when the overgrowth of Candida is cured and then begin to treat the Leaky Gut. The diets for each are totally different. I hope you can shed some light on this situation. Thanks
I found out 3 years ago that I had candida overgrowth – I had been struggling with weight, health and anxiety issues. I had been given a constant stream of antibiotics from the age of 3 months old, coupled with a high sugar diet left me very large, depressed and incredibly unhealthy. After starting a low sugar diet I lost alot of weight and reigned in my sugar addiction but have never been able to put anything back into my diet due to an immediate reaction (I am now 40) After reading your updates – I now understand what is happening, I take grapefruit seed extract, good pro biotics and keep within a very strict guideline for my diet. Its been a long road and an even longer one stretching out in front of me – but I am more positive and have an understanding – thank you.
I am now in my 47th day of Candida Diet and am feeling great! I wanted to know if I can now take food supplements and vitamins? can it go together with the treatment? I will be eagerly waiting for your reply. Thanks and more power!
Yes you certainly can! Just make sure that you read the ingredients carefully and check that there is nothing that might worsen your Candida.
I would like to add that I also have diabetes and this might be the big factor why I had a candida overgrowth. I don’t want to stop with the diet since it has helped me a lot and I know that am not completely healed yet, besides, I have lots of recipes to make the diet attractive. Thanks again. . .
I find that it takes 4 weeks of eating sugar to create a candida problem, and just 2 times of deep fried food, even a week apart, to get candida
I’ve been doing some research on the significance of high fat intake on the inhibition of proper insulin function (which basically means your blood sugar stays high longer than it should after a meal and feeds candida). Pretty interesting stuff. May explain the fried food problems!
Are you saying, stay away from fat?
I have found some very useful information on this website and I would like to try the diet. Please can you tell me if the diet plan caters for vegetarians?
Yes it certainly does! You need to make some small adjustments to ensure that you are getting enough protein, but it can definitely be followed by vegetarians.
I believe this is the most interesting and informative update about candida and why it can not be easily eliminated.I just have one question. Are these biofilms destroyed by natural antifungals like oregano oil,caprylic acid etc..? Or are the natural antifungals making the biofilms resistant as well?looking forward for your answer!!
Natural antifungals can destroy biofilms given enough time, but they are much more effective when combined with a low sugar diet and probiotics.
What probiotic should be used to help restore the good bacteria and eradicated candida? Pls advise
Hi Jetti, you can see the probiotics that I recommend here.
Hi Lisa,
All your information is so helpful. I’ve been dealing with Candida for the past 15 years and it has slowly gotten worse. The past year I have been on different prescription antifungals along with herbal antifungals and a very restrictive candida diet. My blood work has shown no change in my yeast levels, chronic, acute or GI systemic. Very upsetting but I’m not giving up. I had just recently read about biofilm on Candida just before your article came out. I’m not sure of the safety but due to frustrations I have started taking 3 drops of Tea Tree essential oil in a pint glass of water each day. I have also started 2 drops of clove and 2 of lemongrass essential oils because I found research that showed them to be effective with removing biofilm. Have you come across this in your research.
Thanks
Both clove and lemongrass have antifungal properties, however you don’t mention probiotics – adding some good quality probiotics will make your treatment much more effective!
I have been left feeling worse off after being prescribed about eight different types of antibiotics (amongst other medicines) over the past two years! If only I had known the effects before taking them! I am slowly changing my diet to prepare for the Candida Diet but I haven’t started the plan yet. I have now been prescribed Itraconazole although I have not been tested for any condition. The leaflet shows this medicine has lots of side effects. Do you think it is a good idea to take it? I am worried about the effects it may have on my cells and liver. Maybe it would be ok to take it once I have started the diet? Please can I have some advice?
I’ve have been dealing with candida systemic infections since 2008 after using antibiotic. I felt horrible! It was left untreated for MONTHS. Until I went to an ENT who then put the scope up my nose and down my throat and said my throat was covered in geen mold from yeast. Has severe pain on right side of neck. He gave me a script for Nystain and the main symptoms went away but I’ve had nasal drip for 8 years since. Also I could not drink wine or alcohol without my knees burning had bloating after eating even the smallest meal, could not lose weight no matter how long I exercised. So since then I recently had another flare up of margarine, burning mouth, cracked skin on corners of mouth, brain fog, can’t remember anything, ear pain/pressure, in and out of the ER 4 times because the pain on the right side of neck moved to soft palette (above in my sinus) after being prescribed diluflican. I’m thinking that initial neck pain which felt as though it was my jugular vain may have been a biofilm attached. Then the anti fungal medicine (diluflican) made it move to the sinuses? I’m not sure but since then I still feel a lump in soft palette. I had 2 CT scans and an MRI and it shows nothing. I’m afraid to take more diluflican as I’m worried where else can this lump move to? Can the biofilm move to my brain? I’ve been on yeast diet for 2 weeks now and it helps with ear pain and migraine. You can not cheat! I made a mistake and ate a piece of cantaloupe and started right back at square one. Immediately the symptoms came back. My advise to anyone suffering for extreme yeast flare up is start with nystatin or diluflican ( Fluconazole ) you can buy it online at Fludan.com. (Canadian pharmacy) I’m in the US and it’s not available w/o prescription here. Start with those meds and continue on the yeast doet for as long as you can then slowly start to add foods back. I’m just starting to feel normal again.
I think the anti-candida diet is a very good place to start off if you are experiencing all the “candida overgrowth” symptoms but if you’re finding it isn’t helping you I would definitely look into getting your blood tested for things like Rickettsia, Microplasma, Chlamydia-Pneumonia, Lymes, Babesia, Bartonella and Bilharzia. These are all parasites caused by ticks, fleas and mites. My brother has been dealing with a few of these for about 5 years and has really bad brain-fog, chronic fatigue and many other symptoms. Maybe this can help some of you. Also have just discovered upon biofilms and are hoping to get rid of these in his body so that the parasites can actually be attacked.
I’m so glad I found this site. When I share with my husband my symptoms he thinks I’m loosing it! For me the die off symptoms have been very intense, my liver seems to have a hard time processing all the toxins. I pray each and everyone of you recover fully and quickly from this pest 😔 I remind my self to keep a positive mindset thru this journey. God bless you all.
Ditto! I just had mesh removed and now the overgrowth of candida is horrible. Inflammation is 7000! I feel so tired and my liver is also having a hard time. I believe God had me find this site. Not sure if you tried this or not, but I’d love to hear from you how you are better! 🙂
The most effective treatment for candida, crohns, UC and IBD is to eat a whole food plant based diet while intermittent fasting. Use a 4-6 hour feeding window. Lately my meals have consisted of strawberries, blueberries, bananas, fresh lemons and limes, green veggies, and black beans mixed with sauerkraut. I noticed a HUGE difference after I started eating 1 raw garlic clove a day. I have a hard time believing the probiotic supplement I’m taking is making any positive impact but I decided to include it anyways. Once I felt 100% and started seeing normal brown sausage-like stools for a couple days I performed a test and started drinking a couple rum and cokes every day and eating tons of sugar in the form of cakes, cookies, brownies while cutting out the garlic. It took approximately 7 days to get back into a state where I felt extreme fatigue with gut inflammation and pain where I couldn’t take it anymore and needed to get back to eating clean once again. My stools obviously were not normal brown sausage-like stools anymore at this point. After approximately 7 days of eating clean with garlic I was able to get back to feeling fully energized while experiencing no gut inflammation or pain. The human body is amazing at healing itself when you give it what it needs.